Local Guide — Park Ridge, IL
TRIGGER POINT THERAPY IN PARK RIDGE
Targeted treatment for muscle knots and referred pain. Manual release, dry needling, and IASTM with Dr. Gontarek. BCBS PPO accepted.
Medically reviewed by Missy Zammichieli, DNP, APRN, FNP-BC · Treatment by Dr. Michael Gontarek, DC, MSc, DACBN · Updated April 30, 2026

From the Provider
Missy Zammichieli, DNP, APRN, FNP-BC
Doctor of Nursing Practice
Board-Certified Family Nurse Practitioner
One of the most underdiagnosed problems I see in primary care is myofascial trigger points. The patient presents with chronic tension headaches, or shoulder pain that radiates down the arm, or low back pain that sends symptoms into the hip. They've had imaging, sometimes multiple rounds, and the imaging is clean. Their PCP is now reaching for muscle relaxants or considering pain management referrals. Meanwhile the actual driver — a hyperirritable knot in a specific muscle that's referring pain elsewhere — has never been properly assessed.
Quick clarification on terminology, because the page URL says "trigger point injections" and we want to be honest with patients searching for that. There are three closely related treatments people lump together: manual trigger point therapy (sustained pressure), dry needling (a thin filiform needle, no medication), and trigger point injections (a small amount of local anesthetic injected by an MD/DO/NP). At Moonshot, Dr. Gontarek performs manual trigger point work, dry needling, and IASTM. We don't currently offer anesthetic-based injections — for most patients, dry needling produces equivalent results without the medication.
What I see referred to Dr. Gontarek most often: tension headaches that originate at the upper trapezius and suboccipitals; "rotator cuff" shoulder pain that's actually infraspinatus trigger points referring forward; piriformis-driven sciatica-like leg pain in patients with clean lumbar imaging; and TMJ-style jaw pain driven by chronic clenching of the masseter and temporalis. All of these are mapped, well-documented referral patterns. Once you know the map, finding the source is fast.
My honest take: if you've been chasing pain at the location it shows up — neck for headaches, shoulder for shoulder pain — without a structured trigger point assessment, you may have been treating the wrong site for months. Most patients who come here with "I've tried everything" feel meaningful improvement after one or two visits, because nobody had ever properly examined the actual pain generator.
WHAT ARE TRIGGER POINTS?
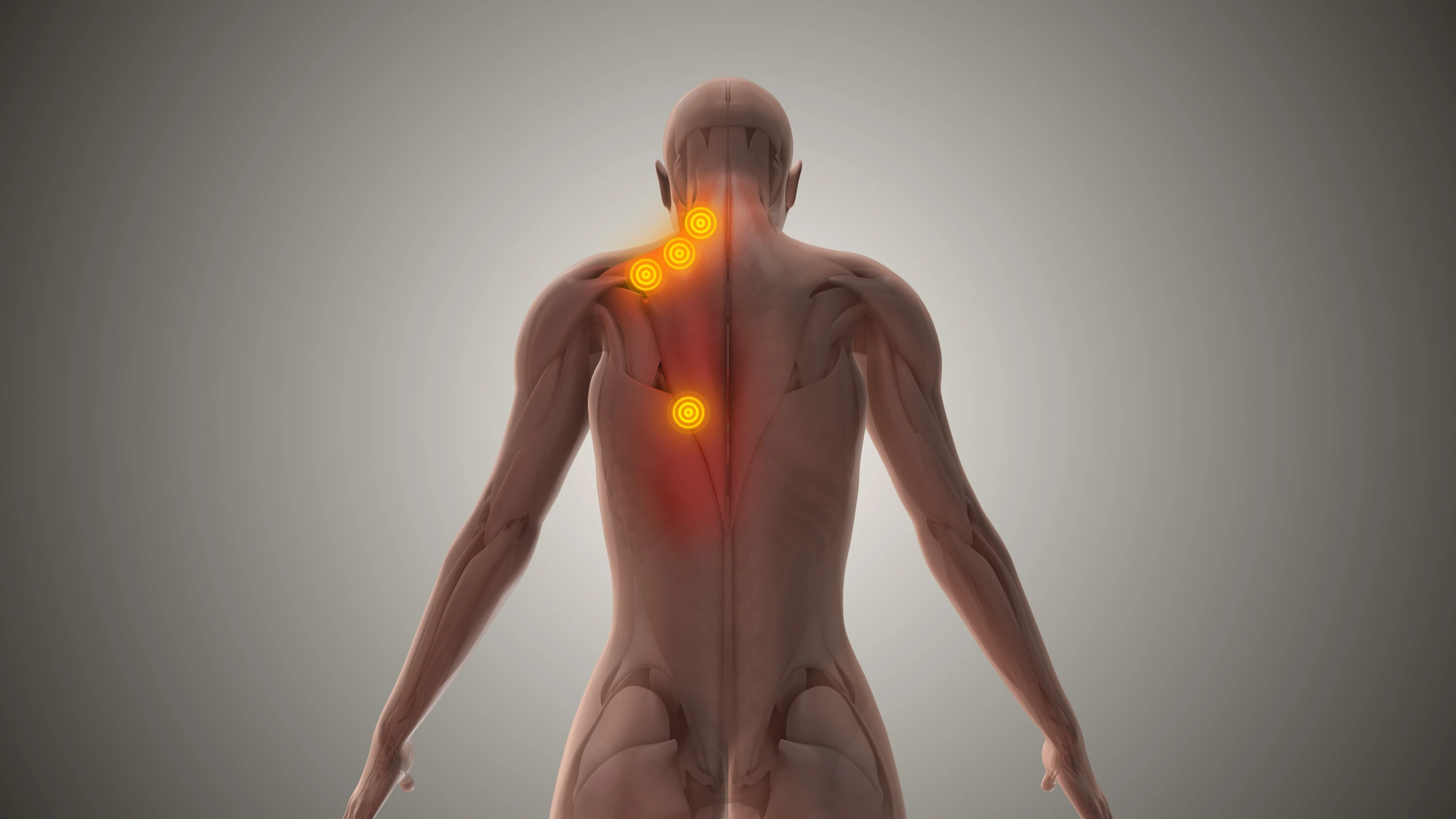
A trigger point is a hyperirritable spot within a taut band of skeletal muscle. If you've ever felt a tight "knot" in your neck, shoulder, or back that's painful to the touch and seems to send pain somewhere else when pressed, you've felt an active trigger point.
These aren't just tight muscles. Trigger points are localized areas where muscle fibers are stuck in sustained contraction at the microscopic level. The fibers can't release on their own because they're locked in an energy crisis: the contraction restricts local blood flow, oxygen drops, metabolic waste accumulates, and the muscle lacks the energy to let go. The result is a self-perpetuating cycle of contraction, ischemia, and pain.
What makes trigger points distinctive is referred pain. Unlike a bruise or a strain that hurts right where the injury is, trigger points send pain to other areas of the body in consistent, well-mapped patterns. This is why so many people chase the wrong source for months. You treat where it hurts, but the pain generator is somewhere else entirely.
Why this matters: A trigger point in your upper trapezius can cause a headache. A trigger point in your infraspinatus can cause shoulder and arm pain that mimics a rotator cuff injury. A trigger point in your piriformis can cause sciatica-like symptoms down the leg. If you've been treated for the symptom location without relief, the actual source may be a trigger point referring pain to that area.
COMMON TRIGGER POINT REFERRAL PATTERNS
Trigger points in one muscle send pain to a completely different area. These patterns are consistent and well-documented, which is what makes them identifiable and treatable.
Upper Trapezius
Refers to: Head & Temple
The most common trigger point location. Knots in the upper trap refer pain up the side of the neck and into the temple, causing tension headaches. If you get headaches that start at the base of your skull or behind your eye after long hours at a desk, upper trap trigger points are a likely culprit.
Infraspinatus
Refers to: Shoulder & Arm
A rotator cuff muscle on the back of the shoulder blade. Trigger points here send deep, aching pain into the front and side of the shoulder and down the arm. This pattern is frequently mistaken for rotator cuff injury, frozen shoulder, or even biceps tendinitis.
Piriformis
Refers to: Buttock & Leg (Sciatica-Like)
A deep hip rotator that sits directly over the sciatic nerve. Trigger points in the piriformis can compress the nerve and send pain, tingling, or numbness down the back of the leg. This mimics true sciatica from a disc herniation but originates from a muscular source.
Quadratus Lumborum (QL)
Refers to: Lower Back & Hip
A deep core muscle connecting the pelvis to the lowest rib. QL trigger points refer pain across the lower back, into the hip, and sometimes into the buttock. This is one of the most common sources of chronic low back pain that doesn't show up on imaging.
Sternocleidomastoid (SCM)
Refers to: Face, Ear & Eye
The large neck muscle that runs from behind your ear to your collarbone. SCM trigger points can cause frontal headaches, ear pain, jaw aching, and even dizziness. These are often misdiagnosed as sinus headaches or inner ear problems.
Masseter & Temporalis
Refers to: Jaw, Teeth & Temple
The primary chewing muscles. Trigger points from jaw clenching, teeth grinding, or stress refer pain into the teeth, ear, and temple. Often misdiagnosed as dental problems or TMJ disorder alone. Treating the muscular trigger points can dramatically reduce jaw pain and headaches.
TREATMENT TECHNIQUES AVAILABLE
There's no single "best" approach for every trigger point. Dr. Gontarek matches the technique to the specific presentation, severity, and patient preference.
Manual Trigger Point Release
Sustained, targeted pressure applied directly to the trigger point using thumb, finger, or elbow. The provider isolates the taut band, locates the nodule, and applies progressive pressure until the tissue releases. This is the foundation of trigger point therapy. It's more targeted and diagnostic than general massage because the provider is following specific referral patterns to find the source of your pain, not just working on the area that hurts.
Dry Needling
A thin filiform needle is inserted directly into the trigger point to mechanically disrupt the contracted fibers. The needle breaks the contraction cycle at the motor endplate and often produces a local twitch response, a brief involuntary contraction that signals the trigger point has been hit and deactivated. Dry needling reaches deep trigger points that manual pressure can't fully access. It's especially effective for chronic, stubborn knots. Read our full dry needling guide.
Instrument-Assisted Soft Tissue Mobilization (IASTM)
Specialized stainless-steel instruments are used to detect and treat soft tissue restrictions, fascial adhesions, and trigger points. The instrument amplifies the provider's ability to feel tissue texture changes and delivers targeted shear force to break up fibrotic tissue. IASTM works well for superficial trigger points, fascial restrictions surrounding the trigger point, and areas where the trigger point sits within a broader pattern of soft tissue dysfunction.
Targeted Stretching & Corrective Exercise
After the trigger point is deactivated, the muscle needs to be restored to its full resting length. Targeted stretching immediately after treatment locks in the release and prevents the fibers from re-contracting. Corrective exercises address the underlying cause: weak opposing muscles, poor posture, movement compensations. Treatment without follow-up rehab is a temporary fix. Treatment with corrective work is a lasting one.
Combined approach: Most sessions use a combination of these techniques. A typical visit might start with manual palpation to identify active trigger points, dry needling or IASTM to deactivate them, then stretching and corrective exercise prescription. The specific mix depends on what your tissue needs that day.
TRIGGER POINT THERAPY vs. INJECTIONS vs. DRY NEEDLING vs. CHIROPRACTIC
These terms get confused constantly. Quick honest comparison:
Trigger Point Injections (TPIs)
A small amount of local anesthetic (lidocaine, sometimes saline or a low-dose steroid) is injected into the trigger point. Performed by an MD, DO, NP, or PA. Mechanism is partly anesthetic and partly mechanical disruption from the needle itself. Outcomes are well-documented. Insurance often covers them when billed by an MD/DO. We don't currently offer TPIs at Moonshot — for most patients, dry needling produces equivalent or better results without medication.
Dry Needling
A thin filiform needle inserted into the trigger point — no medication. Works by mechanically disrupting the contracted muscle fibers and triggering a local twitch response. Performed by Dr. Gontarek at Moonshot. Strong evidence base for trigger point deactivation. The "no medication" piece matters because there's no risk of anesthetic side effects, no concern about repeated steroid exposure, and you can needle as many trigger points in a session as needed.
Manual Trigger Point Therapy / IASTM
Sustained pressure or instrument-assisted shearing applied directly to the trigger point. Best for surface-accessible trigger points, patients who don't want needles, and as an adjunct to other techniques. Less effective than dry needling for deep, chronic trigger points but excellent for the majority of presentations.
Chiropractic Adjustment
Different mechanism — chiropractic addresses joint mobility and segmental dysfunction. Often complements trigger point work but isn't a substitute. Many patients benefit from both: the adjustment restores joint motion, the trigger point work releases the muscular guard pattern that was driving dysfunction. Dr. Gontarek incorporates both when appropriate. See our chiropractic guide.
WHAT TO EXPECT
Assessment & Diagnosis
Dr. Gontarek will take a detailed history of your pain: where it is, when it started, what makes it better or worse, and what you've already tried. Then he'll palpate the muscles, following the referral maps to trace your pain back to its source. When he finds the trigger point, you'll recognize it immediately because pressing on it will reproduce your familiar pain pattern. That "yes, that's it" moment is diagnostic.
Treatment
Based on what's found, the provider selects the appropriate technique or combination: manual pressure, dry needling, IASTM, or all three. Most patients describe the sensation as "good pain" or "hurts so good." It's a deep, satisfying ache that feels productive, not harmful. If dry needling is used, you may feel a brief twitch response. Treatment is more targeted and intense than a massage, but sessions are typically 20–30 minutes, not an hour.
Immediate After-Effects
Many patients feel significant relief immediately after the session. The muscle feels looser, range of motion improves, and the referred pain diminishes or stops entirely. Some soreness at the treatment site is normal for 24–48 hours, similar to the feeling after a deep tissue massage. Drink water, move gently, and avoid heavy loading of the treated area for a day or two.
Follow-Up & Prevention
Some patients resolve completely after one session. Chronic or recurring trigger points may need several sessions spaced 1–2 weeks apart. Your provider will also prescribe specific stretches and corrective exercises to address the root cause that created the trigger points: posture, movement patterns, workstation setup, or training load. The goal is to fix the problem, not create dependency on treatment.
WHEN TRIGGER POINT THERAPY ACTUALLY MOVES THE NEEDLE
Trigger point work is most useful in these specific scenarios. If your pain doesn't fit one of these patterns, we'll tell you on the first visit.
1. Chronic tension headaches not responding to medication
Tension headaches that hit by 2pm every desk-work day, that respond partially to ibuprofen but never fully clear, and that recur every week. Almost always driven by upper trapezius and suboccipital trigger points referring pain up into the head. One or two well-targeted sessions plus a corrective workstation setup typically reduces frequency dramatically.
2. Shoulder pain with clean MRI
Patient presents with classic "rotator cuff" symptoms — deep aching, pain reaching overhead — but the MRI is unremarkable. Common cause: infraspinatus or subscapularis trigger points referring pain that mimics a structural shoulder problem. Imaging is clean because the problem is muscular, not structural.
3. "Sciatica" without lumbar pathology
Pain, numbness, or tingling down the leg, but the lumbar MRI is clean — no disc herniation, no significant stenosis. Frequent driver: piriformis syndrome from a deep gluteal trigger point compressing the sciatic nerve. Responds well to a few sessions of dry needling and targeted hip rehab.
4. TMJ / jaw pain with normal dental exam
Patient sees a dentist for jaw pain, gets fitted for a night guard, but the pain persists. Often the masseter and temporalis muscles are loaded with chronic trigger points from clenching, and the night guard alone doesn't address them. Targeted trigger point work on the chewing muscles dramatically reduces residual pain.
INSURANCE, PRICING & ACCESS
Insurance & Payment
- BCBS PPO accepted — in-network for chiropractic and rehab services
- Cash pricing — typically $150 per visit; clear rates, no surprise bills
- Superbills provided — for out-of-network insurance reimbursement
- No referral needed — book directly online
- HSA/FSA accepted
Your Provider
Dr. Michael Gontarek, DC, MSc, DACBN is a chiropractic physician with advanced credentials in clinical nutrition and musculoskeletal rehabilitation. He combines manual therapy, dry needling, and instrument-assisted techniques to treat trigger points and the movement dysfunctions that create them.
Evidence-based care, no long treatment plans you don't need. The goal is resolution, not retention.
WHAT PARK RIDGE PATIENTS SAY
Real reviews from our Google Business Profile.
"Daily tension headaches for three years. Tried PT, massage, three different meds, even Botox. One dry needling session targeting my upper traps and suboccipitals and the headaches dropped from daily to weekly. Two more sessions and they're basically gone."
— Patient, Park Ridge
"Shoulder pain for eight months that two orthopedists said was 'probably impingement, just rest it.' MRI was clean. Came here, Dr. Gontarek found a massive infraspinatus trigger point in 30 seconds — the moment he pressed on it I recognized exactly the pain I'd been chasing. Three sessions later, gone."
— Patient, Glenview
"Diagnosed with 'sciatica' and was told I might need an epidural. MRI showed nothing significant. Dr. Gontarek treated my piriformis with dry needling and gave me a hip mobility program. Symptoms resolved in two weeks. Saved me a series of injections I didn't actually need."
— Patient, Niles
CONDITIONS WE TREAT WITH TRIGGER POINT THERAPY
Tension Headaches
Trigger points in the upper trapezius, suboccipitals, SCM, and temporalis are one of the most common causes of tension-type headaches. If your headaches start at the base of your skull, behind your eyes, or at your temples after desk work or stress, trigger point therapy can often reduce their frequency and intensity dramatically.
Neck & Shoulder Pain
Desk work, phone use, and driving create chronic tension in the upper traps, levator scapulae, and scalenes. These trigger points cause stiffness, restricted range of motion, and pain that radiates into the arm or hand. This is the most common presentation we treat and one of the most responsive to trigger point therapy.
TMJ & Jaw Pain
Jaw clenching and teeth grinding create trigger points in the masseter, temporalis, and medial pterygoid muscles. These refer pain to the teeth, ear, and temple and restrict mouth opening. Trigger point therapy to the masticatory muscles provides relief that a night guard alone often can't.
Lower Back & Hip Pain
Trigger points in the QL, paraspinals, gluteus medius, and piriformis are frequent contributors to chronic low back and hip pain. These can mimic disc-related symptoms or SI joint dysfunction. Identifying the myofascial component often provides relief that imaging-guided interventions miss.
Sciatica-Like Leg Pain
Not all sciatica comes from the spine. Piriformis trigger points can compress the sciatic nerve and send pain, tingling, or numbness down the leg. If your MRI is clean but you still have leg symptoms, a muscular trigger point may be the actual source.
Chronic Pain Syndromes
Myofascial pain syndrome, fibromyalgia-related trigger points, post-injury muscle guarding, and persistent muscle spasms that haven't responded to stretching, heat, or oral medications. When the pain has been there for months without a clear structural cause, trigger points should be evaluated.
VISIT THE PARK RIDGE CLINIC

Moonshot Medical and Performance
542 Busse Hwy
Park Ridge, IL 60068
- Two blocks east of Lutheran General Hospital, near Busse Hwy & Cumberland Ave
- Free dedicated parking lot on-site
- ~10 min from Cumberland CTA Blue Line; ~5 min from Dee Road Metra
- ~12 min from O'Hare for out-of-town patients
- Wheelchair accessible ground-floor entry
Rehab Hours (Dr. Gontarek)
- Tue-Wed: 8:00am – 1:00pm, 3:00pm – 6:00pm
- Thu: 8:00am – 1:00pm
- Fri: 8:00am – 1:00pm, 3:00pm – 5:00pm
We see patients across the northwest Chicago suburbs — Park Ridge, Des Plaines, Niles, Edison Park, Norwood Park, Rosemont, Morton Grove, Glenview, Skokie, Mount Prospect, and Arlington Heights.
542 Busse Hwy, Park Ridge, IL 60068
Get Directions →COMMON QUESTIONS
Where can I get trigger point therapy in Park Ridge?
Moonshot Medical and Performance is located at 542 Busse Hwy, Park Ridge, IL 60068 — two blocks east of Lutheran General Hospital. Dr. Michael Gontarek offers trigger point therapy including manual release, dry needling, and IASTM. No referral needed. Book directly through our website.
Do you offer trigger point injections (with anesthetic)?
We don't currently perform anesthetic-based trigger point injections. We do offer manual trigger point therapy, dry needling, and IASTM. For most trigger points, dry needling produces equivalent results without medication. If your specific case warrants anesthetic-based TPIs, we'll refer you to a local MD/DO who performs them.
Does Moonshot accept insurance for trigger point therapy?
Yes. We accept BCBS PPO for chiropractic and rehab services, which includes trigger point therapy. We also offer transparent cash pricing and provide superbills for patients with out-of-network plans so you can submit for reimbursement.
How many sessions will I need?
Many patients feel significant relief after a single session. Chronic or deeply embedded trigger points may require several sessions spaced 1–2 weeks apart. Your provider will assess your response and adjust accordingly. The goal is resolution, not indefinite treatment.
What's the difference between trigger point therapy and massage?
Trigger point therapy is more targeted and clinical than general massage. A trained provider identifies the specific hyperirritable spots causing your pain pattern, then uses precise techniques to deactivate them. Massage addresses general muscle tension. Trigger point therapy diagnoses and treats the specific knots that refer pain to other areas. It's more intense, more focused, and typically produces faster results for specific pain complaints.
Does trigger point therapy hurt?
Most patients describe it as "good pain" or "hurts so good." When the provider presses on an active trigger point, you'll feel a deep ache and often recognize it as the source of your pain pattern. Dry needling may produce a brief local twitch response. The discomfort is temporary and is usually followed by immediate relief and improved range of motion.
References
- 1. Travell JG, Simons DG. Myofascial Pain and Dysfunction: The Trigger Point Manual. Vol 1 & 2. Williams & Wilkins; 1983, 1992.
- 2. Alvarez DJ, Rockwell PG. "Trigger points: diagnosis and management." Am Fam Physician. 2002;65(4):653-660.
- 3. Cummings TM, White AR. "Needling therapies in the management of myofascial trigger point pain: a systematic review." Arch Phys Med Rehabil. 2001;82(7):986-992.
- 4. Shah JP, Thaker N, Heimur J, et al. "Myofascial Trigger Points Then and Now: A Historical and Scientific Perspective." PM R. 2015;7(7):746-761.
DONE CHASING THE WRONG SOURCE?
Trigger point therapy finds the knot causing your pain and treats it at the source. BCBS PPO accepted. No referral needed.
Book Consultation